Researchers Use Aerosol Jet 3D Printing to Develop Neuronal Interface
3D printing has been used in the past to help treat degenerative diseases, or at least make it easier to cope with them. In terms of neurodegenerative diseases, implanted prosthetic devices are often used, but adverse biological reactions in host tissues can result in signal failure. it’s important to create tissue that can mimic the mechanical and structural properties of neural implanted devices, and while flexible polymer-based implants have helped to alleviate some injuries, the mechanical stress doesn’t quite match brain tissue. That’s why a lot of research has been conducted about using conductive polymer (CP) composites or conductive hydrogels to coat the devices so the biocompatibility and electrochemical performance of neural electrodes can be improved.
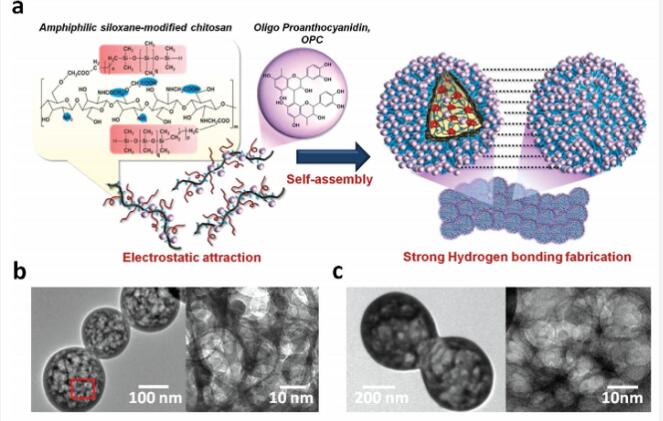 a) Schematic illustration of the mechanism for formation of nanogel-based membrane based on the self-assembly of OPC-incorporated amphiphilic polydimethylsiloxane-modified N, O-carboxylic chitosan (OPMSC), followed by hydrogel-bonding interaction of OPC. The TEM images display the network structure of b) PMSC and c) OPMSC spherical nanogels.
a) Schematic illustration of the mechanism for formation of nanogel-based membrane based on the self-assembly of OPC-incorporated amphiphilic polydimethylsiloxane-modified N, O-carboxylic chitosan (OPMSC), followed by hydrogel-bonding interaction of OPC. The TEM images display the network structure of b) PMSC and c) OPMSC spherical nanogels.
But, a team of researchers from China say that it’s more important to design biocompatible coatings for implanted devices that mimic mechanical and structural properties of brain tissues, so tissue responses after long-term utilization can be reduced.
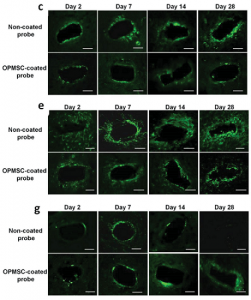
Representative fluorescent images demonstrate tissue responses around the tip of the non-coated probe and the OPMSC-coated probe at days 2, 7, 14, and 28 post-implantation. (c) ED1 staining; (e) GFAP staining; (g) NeuN staining.
The researchers believe that 3D nanostructural coatings should be developed for the insulated regions, and not the implant electrode sites, so implants can interface with nearby brain tissues with more stability. They explained their findings in a recently published paper, titled “Multifunctional 3D Patternable Drug-Embedded Nanocarrier-Based Interfaces to Enhance Signal Recording and Reduce Neuron Degeneration in Neural Implantation.”
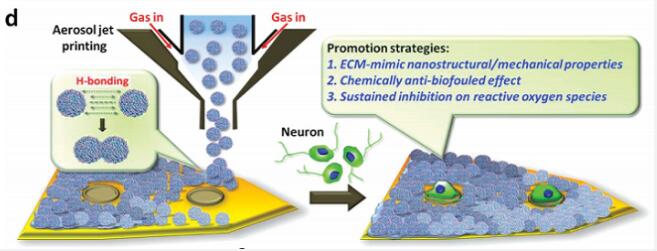
Using aerosol jet printing, the OPMSC suspensions were directly patterned on a neural probe to create an anti-inflammatory neural interface.
The researchers used aerosol jet 3D printing to develop a neuronal interface with prolonged anti-inflammatory ability, structural and mechanical properties that mimicked brain tissue, and a sustained nonfouling property in order to inhibit tissue encapsulation.
They created a new 3D nanocarrier-based neural interface that could possibly be used to support long-term neural implantation, as well as achieve better therapy for chronic and degenerative diseases. The researchers used a “novel combination of antioxidative zwitterionic nanocarriers and nanomanufacturing technology” to make the interface. The team developed a new type of anti-inflammatory nanogel, based on the amphiphilic polydimethylsiloxane-modified N, O-carboxylic chitosan (PMSC) incorporated with oligo-proanthocyanidin (OPC), called OPMSC.
The team directly fabricated OPMSC nanogels onto a membrane using aerosol jet printing technology, because it is a low-temperature technology. When developing neural implants, mechanical properties are the main concern, which is why the researchers conducted a tensile test, among other experiments, on their new 3D nanocarrier-based neural interface, which was also implanted into rodents.
Co-authors of the paper are Wei-Chen Huang, Hsin-Yi Lai, Li-Wei Kuo, Chia-Hsin Liao, Po-Hsieh Chang,Ta-Chung Liu, San-Yuan Chen, and You-Yin Chen.
Source: 3D Print




Recent Comments